Polycystic ovary syndrome (PCOS) - does it make it harder to get pregnant?.
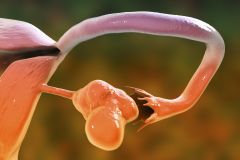
What are polycystic ovaries?
Polycystic ovary syndrome (or PCOS) is a disorder affecting women of reproductive age - according to the Central Statistical Office in Poland, the age range is 15 to 49 years. Polycystic ovaries are characterised by a large number of follicles, visible on ultrasound examination. The mechanism of their formation depends mainly on genetic, endocrine, metabolic and environmental factors.
PCOS can cause infertility in women, due to hormonal disturbances. However, it is not a verdict. According to specialists, with lifestyle changes and appropriate therapy, getting pregnant is relatively high. (1)
Polycystic ovary syndrome - symptoms
PCOS is most often manifested by the occurrence of non-ovulatory cycles and an overproduction of the male sex hormones androgens. Non-ovulatory cycles are a serious obstacle to pregnancy. In addition to this, other menstrual disorders can occur, for example periods that are too frequent or infrequent - at intervals of more than 35 days or less than 21).
Symptoms of polycystic ovary syndrome also include hirsutismThe hair loss in the face (so-called 'male beard'), nipples, groin and back.
Also included are:
- worsening of the skin condition - acne (especially in the jaw area),
- greasy skin and hair, hair loss and male pattern baldness (in the form of "cornrows"),
-
mental deterioration, for example anxiety disorders, depression,
- skin discolouration,
- Weight gain - android type obesity in the abdominal region. It often occurs in combination with insulin resistance, predisposing the patient to the development of metabolic syndrome and hepatic steatosis.
INSULIN RESISTANCE
Polycystic ovarian syndrome often goes hand in hand with insulin resistance. This is a condition in which the body has significantly reduced insulin sensitivity (a hormone that regulates blood sugar levels). Insulin resistance usually leads to a pre-diabetic state and also to the development of type two diabetes. (2)
Polycystic ovary syndrome - treatment
If you have noticed worrying symptoms in yourself, see a gynaecologist or possibly an endocrinologist immediately. The specialist will take a thorough history with you, order tests, make a diagnosis and plan the appropriate treatment. A quick change in lifestyle, diet and introduced drug treatment can relatively reduce the symptoms of polycystic ovary syndrome. In patients diagnosed with insulin resistance, it is very important to implement pharmacotherapy in the form of metformin. Supplements are also recommended, which can restore ovulatory cycles and improve oocyte quality.
Also see your GP, whose job it is to monitor your health on a regular basis. This way, if metabolic changes occur, your doctor will be able to refer you for a consultation with a specialist. If, along with PCOS, you also suffer from insulin resistance and are obese, a visit to a dietician is advisable. On the other hand, if your mental state has deteriorated severely (among other things due to the fact that you are infertile), you feel anxiety, a drop in mood, a lack of strength and a general breakdown - see a psychiatrist or psychotherapist. Remember that this is nothing to be ashamed of.
What does testing for PCOS syndrome look like?
At the very beginning, the gynaecologist carries out a detailed interview with the patient. He asks her about her complaints and the date of her last menstrual period. He then invites her to a chair where he will perform a transvaginal ultrasound examination. This allows her to see the ovaries in detail, i.e. their size and the number of follicles inside them.
According to the International PCOS Network's 2018 guidelines, a polycystic ovary is one with a volume of approximately 10 cc and/or with (but not necessarily) at least 20 follicles between 2 and 9 millimetres in diameter in each organ.
Next, the woman should perform hormonal tests (day 2-4 of the cycle) by means of an elbow vein blood draw. These include measurement of testosterone, SHBG (this is a protein that binds sex hormones), androstendione, dehydroepiandrosterone (DHEA-S), 17OHProgesterone and also the gonadotropins luteinising hormone (LH) and folliculotropic hormone (FSH). There are also tests for progesterone levels (a test performed about seven days after the expected ovulation will help to determine whether the woman's body is ovulating) and a glucose load test - glucose and insulin levels (a two-step, three-step test).
The doctor will also order tests to rule out other endocrine disorders, for example: thyroid disease, congenital adrenal hyperplasia or Cushing's syndrome. (3)
Bibliography
Authorisation of content:
Dr Anna Niesłuchowska-Hoxha, MD - Obstetrician-gynaecologist from the InviMed clinic in Katowice, Poland
The medical information presented should be considered as general guidelines and does not replace the individual judgement of the doctor regarding the medical management of each patient. The doctor, after a thorough examination of the patient's condition, determines the extent and frequency of diagnostic tests and/or therapeutic procedures, taking into account specific medical indications. All medical decisions are made in full consultation with the patient.
Author of the article
Invimed editorial team - we serve patients by solving their fertility problems. We use world medical knowledge, state-of-the-art technology and treatment methods. We are here to make dreams of parenthood come true. The smiles on the faces of happy parents give meaning to our work.
See all articles →